HIGH ALTITUDE FROSTBITE
In the fall of 1943, there was one United States General Hospital in England. This was at Oxford and was staffed by doctors from Columbia University's College of Physicians and Surgeons and Presbyterian Hospital. John E. Scarff, a member of that hospital's staff, was the only qualified and experienced neurological surgeon in the European theater of operations.
The injuries resulting from the activities of the United States Army were confined to traffic accidents, which occurred in the majority of instances at night with jeeps appropriated by soldiers exploring the countryside in search of pubs. The United States Eighth Air Force was active in its attempts to prove the superiority of daylight over night bombing, employed by the British. The officers of the Medical Corps assigned to the Air Force were more active politically in their attempt to establish themselves as the Air Force Medical Corps, separate and distinct from the regular Medical Corps. The Surgeon of the Eighth Air Force, Malcolm Grow, as aggressive in the promotion of this goal. I had precious little to do as the Senior Consultant in Neurological Surgery to the Chief Surgeon of the European theater of operations. This was true of the other consultants removed from the busy life of surgical practice and teaching. It seemed ridiculous to have received a special commendation for the suggestion that keys be removed from the jeeps to prevent nocturnal joy rides with the resultant crashes and skull injuries.
One day, with Barrett Brown, Consultant in Plastic Surgery and Burns, a surgical combination undoubtedly the result of the experience of the British with personnel injured in burning aircraft and requiring surgical restorative procedures, I visited General Hospital No. 2 at Oxford. We were shown an airman who had huge blisters on the dorsal surface of his hands and fingers. We were told by the ward surgeon that these had resulted from a fire that enveloped the crippled aircraft when it returned to its base. Quite by chance, I was the last to leave the bedside when the patient volunteered that he was not burned; his hands had been injured after he removed his gloves to urinate when his B-17 was at an altitude of 35,000 feet and the temperature was -50ş F. The soldier made his own diagnosis of frostbite and was understandably upset that no one had asked him how his injury had occurred, and that false assumptions had been made. He had received a quick freeze of his hands. This was the beginning of my interest in high altitude frostbite.
As the bombing raids over Germany increased in frequency, more frostbite injuries were encountered. The problem was presented to Paul Hawley, Chief Surgeon of the European theater of operations, and he granted permission to have all of the airmen with frostbite injuries admitted to a special ward at the No. 2 General Hospital.
The hands were most frequently involved, but there were several instances of frostbitten buttocks in ball turret and tail gunners. I learned that they flying suits were wired in series for warmth and that if one glove was removed, the circuit for the entire suit was disconnected. The waist gun positions were exposed to the outside environment; pilots and navigators were not among our patients.
At first our treatment was empirical; gradual and rapid reheating methods were contrasted; capillary studies were made; vasodilator drugs were employed; color film was obtained through a British civilian friend to photograph the injuries and results of treatment. Complete casts of the skin of the affected fingers sloughed away, leaving a painful, sensitive, reddish purple skin. The question of interrupting the sympathetic nerve supply to the hands, creating a situation analogous to that in treatment of Raynaud's disease, was considered.
While our basic studies were in progress, more and more frostbit injuries were being examined and treated, and our experience increased. The surgeon to the Air Force actually denied that there were such injuries. I was ordered to present to him the photographic evidence and the data that had been collected. Reluctantly he had agreed to General Hawley's request to hear and see the evidence. Ignored for twenty minutes after being admitted to Colonel Grow's presence upon a prearranged appointment, I stood to leave. I explained that perhaps he might be interested in reviewing the photographs and evidence later, at his convenience. He said that these injuries were minor and that his opinion was based upon his experience in Siberia following World War I. He was surprised when I told him that the flying suits were wired in series, and he denied it. He called Harry Armstrong into his office to refute the statement and was nonplussed when Armstrong calmly stated that he had no idea how they were wired. Grow continued to ignore the high altitude frostbite injuries and oppose our effort; he used his influence to keep us off United States airfields when we wished to inspect the B-17 waist gun positions.
More and more evidence was accumulating and we were learning about the immediate and late treatment of these injuries. General Hawley had called General Henry Arnold's attention to the injuries, and one morning I was requested to accompany Arnold and his staff on hospital rounds. Suddenly we were joined on the ward by Colonel Grow, who explained to General Arnold that he and his medical group had discovered the frostbite injuries, had set up the study, and had recommended steps to be taken for their prevention. My friend Hawley quickly prevented any impulsive or ill chosen remarks on my part and drew me aside saying, "Loyal, I have served with Hap Arnold in many places; in fact, I have taken care of his children. He's no fool."
Soon thereafter, I was ordered to Washington to present all the data to Surgeon General Kirk, who gleefully, it seemed to me, sent me to the Air Surgeon's office to present the color photographs and the results of the clinical investigation. As a result, the waist guns were enclosed in Plexiglas for protection of the waist gunners, and the electrical wiring of the flying suits was redesigned. The independence of the newly established Air Force Medical Corps was not seriously impaired.
With few exceptions, injuries to airmen, infantrymen, and sailors are similar surgically and are treated in the same way. Why should there not be a medical corps for the armed services, instead of three separate organizations with duplication of hospitals, supplies, and personnel? The only reason, it seemed to me, was the selfish desires of men to establish their own empires.
This article was the first description of frostbite produced by low temperatures at high altitude. It called attention to the fact that trench foot and immersion foot were other examples of cold injury, and that the effects were evidence of the length of exposure, the temperature of exposure, and the wetness or dryness of the environment. Perhaps it contributed to the productive experimental and clinical investigations of cold injuries that followed. Certainly it provided insight into the ramifications of military medicine and the bitter service rivalries that existed among professional military personnel. But more important, it emphasized the necessity of listening to and evaluating the patient's story before making a diagnosis. Over the years I have obtained satisfaction and pleasure from the basic work we did on this problem, and I know that our men in three recent wars have benefited from this effort.
LOYAL DAVIS

HIGH ALTITUDE FROSTBITE
LOYAL DAVIS, M.D., F.A.C.S., Colonel, M.C., A.U.S., Chicago, Illinois
JOHN E. SCARFF, M.D., Major, M.C., A U.S., New York, New York
NEIL ROGERS, M.D., Major, M.C., A.U.S., Oxford, England
MEREDITH DICKINSON, M.D., Lieutenant, M.C., A.U.S., Rochester, New York
Cold damage to the extremities suffered by the high altitude airman is unique among injuries of thermal origin. It differs from the common frostbite as greatly as the "Bird's Eye" frozen foods differ from cold storage foods. One fundamental fact is common to these injuries, to the frostbite incurred by ground troops during severe winter weather, and the immersion foot of shipwrecked seamen; namely, that the primary agent which produces the pathologic changes in the affected tissues is cold.JOHN E. SCARFF, M.D., Major, M.C., A U.S., New York, New York
NEIL ROGERS, M.D., Major, M.C., A.U.S., Oxford, England
MEREDITH DICKINSON, M.D., Lieutenant, M.C., A.U.S., Rochester, New York
The secondary mechanisms, however, which operate to make the tissues particularly vulnerable to cold differ between common frostbite, immersion foot, and the frostbite of the high altitude flyer; and in the latter case are, in many respects, unique.
In high altitude frostbite, for example, extreme degrees of cold (-40 to -52ş C.) are encountered. The effect of these low temperatures upon the tissues of the extremities is further augmented by varying degrees of anoxemia and ischemia. In the frostbite incurred by ground troops the flat surfaces of the face and of other exposed portions of the body, as well as the extremities may be attacked; whereas, in high altitude frostbite one of the most striking features is the predilection for the extremities. In immersion foot, the degree of cold is moderate in comparison and the secondary factors are venous stasis, maceration of the skin by sea water, infection of the soft parts introduced through the macerated skin, malnutrition, and lowered general vitality due to sheer physical exhaustion. In the frostbite of the high altitude flyer the exposure to cold may last only a few minutes, whereas in the frostbite of ground troops or the immersion foot of the seaman, the exposure to cold may be for days or even weeks.
CLINICAL TYPES
Mild type. It is quite common to find that an airman removes his gloves in order to make some necessary adjustment of his equipment. This may require only a minute or two. However, during this brief time the fingers become painfully cold, numb, stiff, waxy white in appearance, and completely insensitive to touch. They feel hard and even brittle when palpated and if the fingers are struck against a hard object, the sound produced is similar to that which would follow if a piece of wood were struck against the same object. The fingers cannot be flexed or extended voluntarily and often are so stiff that they cannot be moved with the other hand.Recovery from this condition may be quite slow, even after removal to a warmer environment, and quite often hours elapse before the tips of the fingers begin to soften. Even after the tissues become less hard and approach normal, the waxy or ashen white ischemic appearance may persist for several more hours (Fig. I). The surface temperatures, as recorded by thermocouples attached to the finger tips, may be 4 to 6 degrees (C.) colder than the corresponding fingers of the unaffected hand. Capillary microscopy of the affected fingers at this early stage shows no blood whatever in the terminal capillaries on the dorsum of the fingers about the nail beds (Fig. 2). This would appear to be the result of an initial intense vasomotor spasm of the terminal portions of the arterioles and, in some instances, to a secondary thrombus at the point where the arteriole, with its muscular wall, passes into the thin-walled capillary. These findings will be presented in detail in the discussion of the pathology to follow.
If at this stage, the individual's extremities and body can be brought back to the normal body temperature, no permanent ill effects may result. His fingers, however, may ache and throb for several hours and paresthesia may persist for days or weeks but there will be no blistering, gangrene, or other gross anatomical residuals.
Severe types. If the exposure to cold is prolonged, permanent damage to the tissues of the extremities will occur and definite clinical manifestations of severe damage become apparent. These sequelae follow two patterns which for convenience may be described as the "wet" and the "dry" forms. The fundamental pathology of the two types is essentially the same.
In the wet type, multiple small cutaneous blisters appear rather simultaneously upon many points of the skin of the affected part which rapidly grow in size and coalesce to form one or several huge blisters involving the dorsum of a finger, or even the dorsum of the entire hand. These may be similar to the simple vesicles incurred in second degree burns, and contain free fluid, but more often the blisters differ from the blisters of burns in that the pathologically excessive fluid is held fast within the tissue composing the superficial layers of the skin. The blisters may have the appearance of simple vesicles containing free fluid, but if an attempt be made with a syringe and needle to aspirate the fluid, none, or only a very small amount, can be obtained (Fig. 3a). However, fluid will slowly ooze from the needle puncture holes for many hours. This fluid may be a clear transudate (Fig. 4a) or it may contain blood corpuscles (Figs. 5a, b). The latter rapidly turn a dark color and impart to the affected parts an appearance easily mistaken by the uninitiated for gangrene (Fig. 15a). This dropsical condition tends to persist for 2 or 3 days after which the fluid disappears and the superficial layers of the skin become loose and wrinkled, then dry and hard.
Hemorrhage usually takes place beneath the nails giving them the same appearance as a nail which has been crushed and, in such cases, the nail is lost.
In both the simple vesicles and in the dropsical blisters, the superficial layers of the skin are dissected away from the deeper layers by extravasated fluid. When this skin dries and hardens it is cast off, frequently in the form of a complete cast of the part (Fig. 7). The separation occurs just beneath the basal germinal layer of the epithelium so that the greater part of the germinal layer comes away with the cast (Fig. 8). Epithelial regeneration later on is possible, therefore, only from the remnants of the germinal epithelium remaining in ducts of the sweat glands in the same manner as re-epithelization occurs at the site from which split thickness skin grafts have been taken.
The newly regenerated skin is thin, tightly drawn, smooth, shiny, and varies in color from a dusky pink to a dusky blue (Fig. 3b). The exact color fluctuates freely from one extreme to the other with changes in the temperature of the environment. The part is extremely sensitive to cold. On cool mornings the fingers have a dusky blue color, feel cold, and are painful. As the environment and the patient's own body warm up, the fingers tend to become pink in color, warm, and free from pain. This reflex warming, however, is never as great as in the normal hand. Cold tolerance is strikingly reduced. Whereas the normal hand placed in an environment minus 20 degrees centigrade will resist freezing for over an hour, the hand which has been frostbitten, placed in the same environment will freeze within 10 to 20 minutes (Fig. 9).
After periods of time varying in individual cases according to the severity of the injury, the skin gradually resumes a normal appearance, normal subjective and objective reactions to environmental cold, and the capillary loops slowly regenerate. However, this requires months and, in some of the cases studied, complete anatomical and physiological recovery of the skin to normal has not occurred after 8 or even 10 months.
Anesthesia or hypesthesia to pain and touch is always present to some degree in the affected extremities and commonly extends well proximal and beyond the areas of apparent damage to the skin itself (Fig. 10). These changes may persist for months (Fig. 4b).
Loss of sweating usually occurs in the same areas as the impaired sensation and lasts as long as the sensory loss continues (Fig. 4b).

Fig. 5.a, Hemorrhagic blisters in a moderately severe frostbite. Note discoloration of the nails. b, Same hand 10 days later. The blisters have dried up and the skin has an ecchymotic appearance. Desquamation occurred later.
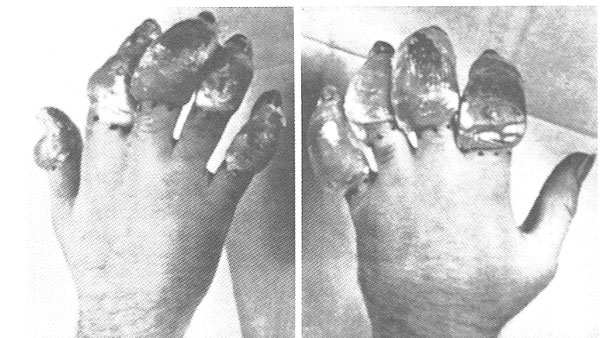
Fig. 6. Photograph showing example of severe hemorrhagic blistering in the wet type of high altitude frostbite 24 hours after injury.
The dry type of high altitude frostbite is usually associated with a more severe exposure to cold. In its initial stage it is indistinguishable from the wet type. The extremities may be literally as hard as rock and require longer to thaw out. At about the time that blisters would appear in the wet type, none develop in the dry type. Instead, the affected parts become very tense, the skin assumes a dull ground glass appearance (Fig. 11a) and the deeper tissues take on a dusky gray color which gradually becomes darker and darker. As time goes on the skin becomes quite dry and the deeper tissues become darker and darker (Fig. 12a, b, c). All the tissues shrivel and mummify and eventually become completely hard and coal black (Fig. 13a, b). These changes are always more marked at the distal end of an extremity; the proximal phalanx is never involved unless the more distal ones are affected. Demarcation between the black, dry, mummified distal portion of the finger and the vital tissue becomes sharp, usually after 2 or 3 weeks. Spontaneous natural amputation will take place if time is allowed, but this process is usually hastened by surgical intervention (Figs. 14a, b; 15a, b; 16a, b; 17a, b, c).
PATHOLOGY
From a pathological viewpoint, the most striking feature of high altitude frostbite is the fact that whereas the face may be exposed to severe cold for several hours without apparent damage, exposure of the fingers to the same degree of cold for only a few minutes may produce damage to tissue so great that gangrene and loss of fingers will result. It must be assumed that the inherent tolerance for cold in a warm blooded animal having a relatively constant body temperature is essentially the same for all tissue cells. It is difficult to explain the great difference in cold tolerance between the tissues of the cheek and the fingers upon the basis of the greater heat radiating surface of the fingers. The heat radiating surface per tissue mass in the fingers is three to four times greater than in the cheek but the susceptibility to cold is fifty to one hundred times greater. Therefore, contributing mechanisms secondary to the primary action of cold on tissue cells must be sought for.Generalized anoxemia, when it occurs, undoubtedly plays a major role in the production or augmentation of tissue damage due to cold in high altitude frostbite, but its effects cannot possibly be selective for tissues in one part of the body.
Localized anoxemia resulting from the ischemia produced by intense reflex vasospasm of peripheral arterioles is undoubtedly the most important factor in establishing the peculiarly selective effect of cold upon the digits of both upper and lower extremities.
Acute peripheral vasoconstriction of the vessels in the extremities occurs almost simultaneously with the exposure to cold. It takes place principally at the terminal end of the arterioles. Direct microscopic examination of the terminal capillary beds in the finger tips soon after they have been exposed to intense cold has revealed the peripheral ends of the arterioles well filled with blood but the terminal capillary loops are entirely empty (Fig. 2). The evidence thus far obtained indicates that this vasoconstriction may persist for 24 hours or longer.
The basic morphological lesion in high altitude frostbite consists of damage by cold to the endothelium of the terminal capillary loops. In mild cases this results only in a pathologic permeability of the capillary walls; but in the more serious cases a thrombus formation occurs at the arteriolar-capillary junction. Under the microscope these thrombi in the terminal stumps of the arterioles are plainly visible (Fig. 2). No thrombosed capillaries have been seen, presumably because early in the train of events they have been deprived of their blood by the intense vasoconstriction which takes place at the terminal ends of the arterioles.
If the vasoconstriction of the arterioles is relaxed before the thrombosis takes place, and the capillary bed is flooded with blood, extravasation of plasma or whole blood may occur through the damaged capillary walls into the tissues. This extravasated fluid may be held within the skin which then assumes a dropsical appearance, or it may collect as free fluid in vesicles. Eventually, the transudate accumulates in the tissue plane between the epidermis and the dermis immediately beneath, or deeper to, the basal germinal layer of cells of the epidermis. The germinal layer and the terminal capillary loops are dissected away from the underlying tissues. Small, irregular capillary loops begin to grow out of the stumps of the thrombosed arterioles after 3 to 4 months but 6 to 10 months may elapse before the appearance of the capillary bed approaches the normal. If a secure thrombosis has developed within the vessels at the arteriolarcapillary junctions before the release of the vasospasm, then the extravasation and blistering do not follow.
If the damage extends more deeply to affect the capillaries beneath the deeper fascia planes which supply muscles and bone, extravasation and hemorrhage occur in these tissues, causing increased tension and severe pain. When thrombosis occurs in the arterioles supplying these deeper tissues, dry gangrene follows. In such cases superficial blistering of the skin may not occur since the blood supply to the skin has been interrupted in the deeper tissues. The clinical picture simply progresses directly from injury by cold to dry gangrene.
The arteries show interesting changes. In 3 cases, requiring amputation of the little finger 3 months after injury from cold, the smaller arteries and arterioles showed a remarkable thickening of the intima which was eight to ten times the normal (Fig. 18). The vessels resembled those seen in cases of endarteritis obliterans. The endothelial lining of the vessels was everywhere intact; no thrombi were seen and nowhere was there a suggestion of recanalization of an earlier thrombus. The mechanisms producing these changes are not clear. However, such changes are said to follow long repeated vasomotor overactivity. The veins were not involved in these pathological changes.
Neural injuries are suggested clinically by the sensory changes in the skin and by the topographical and chronological relationships existing between sensory loss and loss of sweating. Histological studies of nerves have not been successfully made because of the difficulty in obtaining suitable tissue. Whether the loss of sweating is due to local damage to sympathetic nerve fibers or to direct injury to the sweat glands themselves has not as yet been definitely established.
TREATMENT
The treatment of high altitude frostbite must be directed in the first instance to the prevention of these injuries by reducing the necessary exposure to cold and the risks of general anoxemia. These factors are always subject to dislocation in the heat of battle and their reduction falls within the province of the tactician and the engineer.Localized anoxemia of the extremities due to reflex vasospasm is, however, a straight forward medical problem. Its prevention and treatment present a challenge to the physician.
Three types of protective ointments have been studies upon the extremities of normal individuals and patients in whom cold damage has occurred from the viewpoint of preventing the lowering of skin temperature. Careful studies of skin temperature readings after controlled exposures to cold have not yielded results which would indicate that such a line of investigation would prove profitable.
Release of vasoconstriction and its attendant ischemia appear to be a matter of prime importance in the treatment of these cases and must be obtained early if the measure is to be effective; that is, before thrombosis has taken place. Vasodilation may be brought about in the extremities in several ways.
The simplest way to produce vasodilatation is by the local application of heat, but the degree of warmth which should be applied to a frostbitten extremity during the early hours or days of treatment is a moot question. Greene (I) has recommended that the frostbitten extremity be kept at a temperature approximately plus 2 to plus 5 degrees centigrade, because in his opinion (I) heat to the frozen part increases its metabolism and its oxygen requirements and encourages the growth of bacteria and (2) because warmth increases the flow of blood to the part, resulting in greater transudation and blistering. Greene cites Lake's work which showed that the survival rate of tissue cultures is greatest between minus 5 degrees centigrade and plus 5 degrees centigrade.
In line with this reasoning Greene has devised a therapeutic refrigerator (2). It contains one compartment in which solid carbon dioxide is placed and a second compartment into which the frostbitten extremities may be placed. The former communicates with the latter through vents which can be opened and closed as desired to regulate the temperature which is recorded by a thermometer and can be read from outside the box. It is possible to reduce the temperature in the compartment in which the extremities are placed as low as minus 20 degrees centigrade. He advises treatment of frostbitten extremities by placing them in the cabinet with the temperature of the air in the compartment set at plus 2 or 3 degrees centigrade and keeping them there for several days, or even a week, until their removal from the cold cabinet to room temperature is no longer followed by pain in the parts.
We have found Greene's refrigerator an ingenious apparatus and very useful for establishing controlled conditions for studying the effect of cold upon normal and frostbitten extremities. We are not yet prepared, however, to accept without reservation his ideas regarding the therapeutic value of cold in the treatment of the cold damage incurred by high altitude flyers.
It does not necessarily hold that, because temperatures between minus 5 and plus 5 degrees centigrade are optimum for tissue cultures in vitro, bathed with nutrient fluid, the same temperatures are optimum for the metabolism of adult tissue cells in vivo and dependent for their vitality upon the exchange of gases in the circulating blood. Sir Thomas Lewis (3) states categorically, "If the skin is sufficiently cold, 10 degrees centigrade (50 degrees F.) or less, the blood will not part with its oxygen." If we assume Lewis to be correct, it seems illogical to reduce the temperature of the already damaged tissues below 10 degrees centigrade to the levels of 2 to 5 degrees centigrade recommended by Greene. The point stressed by him that the metabolic requirements of these tissues are lowered at the temperature he recommends seems of little consequence in comparison with the fundamental fact that no oxygen is released by the blood to the tissues at these temperatures.
Our studies have shown that great differences in temperature usually exist between the environment and the surface of the extremity. Great variations in these differences of temperature are found between the two hands of the same individual, if one is normal and the other is damaged by cold. Also, great differences between environmental and surface temperatures may be found in the same hand with variations in the general level of the environmental temperature and the duration of exposure to that temperature. Only by taking temperature readings frequently from the skin itself, and preferably with an electric thermocouple, can the actual temperature of the tissues of an extremity be accurately known or even approximately judged. This is all clearly shown in Figure 9. The frostbitten left hand and the normal right hand of a patient were placed in the cold chamber the temperature of which was minus 18 degrees centigrade. The temperature of the affected left hand at the beginning of the experiment was plus 28 degrees centigrade and that of the normal right hand was plus 23 degrees centigrade. Ten minutes later, the temperature of the affected left hand had fallen to plus 1 degree centigrade and that of the normal right hand to plus 18 degrees centigrade. At this point the damaged left hand was removed from the cold box but the normal right hand was kept in the box. Forty minutes later the temperature of the right hand had fallen to plus 6 degrees centigrade, and the temperature of the cold box had risen from minus 14 degrees centigrade to minus 8 degrees centigrade.
It has been noted by many observers, including ourselves, that a frostbitten hand is more apt to blister if it is rapidly warmed or warmed above normal body temperature than if it is kept cool. Greene reasons that this is because with the warming, blood returns in large volume into capillaries whose walls have been damaged and have suffered pathological increase in permeability. Transudation takes place through these damaged walls into the adjacent tissues, thus causing the dropsical and vesicular blisters already described. With this we are in agreement. Greene also believes, however, that the most important objective in the early immediate treatment of the frostbitten hand is to prevent the formation of blisters and he would do this by restricting the quantity of blood flowing into the capillary beds by continuing peripheral vasoconstriction. This vasoconstriction he proposes to obtain by keeping the damaged parts cold; and advises keeping them in a temperature slightly above freezing from the time of injury to as long as several days. We are not prepared to accept this form of treatment at this time.
In an effort to evaluate Greene's recommendations for treatment by continued cooling, we have treated a series of cases by keeping the damaged parts at controlled temperatures approximating those advised by Greene for periods ranging from 24 to 48 hours, after the injury had been sustained. Simultaneously, we have treated a second series of cases by exposing the damaged parts to room temperature, thus allowing a spontaneous refilling of the capillary beds at a natural rate and to a normal degree without attempting to interfere with natural physiological reparative processes. In our judgment, the results obtained by this method were equal or better than those obtained by continued cooling. It is our impression that less blistering occurred in those patients treated by cooling but on the other hand, the patients as a group, complained more of pain and required more sedation that those treated by exposure to room temperature and there was ultimately a greater loss of tissue.
It has been our plan whenever patients were received with two extremities equally damaged to treat one extremity with the continued application of cold and to treat the other extremity by exposure to room temperature. To date we have had only one patient considered suitable for such a controlled experiment. This patient came under treatment soon after he had received cold injury to both hands which to us appeared about equally damaged. Thermocouples were attached to the five digits of his left hand and the extremity was placed in cold packs for 48 hours. Skin surface temperature readings were made every 15 to 30 minutes during this period. The right hand was exposed to room temperature. During the 48 hours of observation the patient complained for more pain in the hand treated by cold than in the other hand. The stages in the subsequent course in the two hands was very similar. Moderate blistering and desquamation occurred in both hands. Following this there was the usual appearance of the remaining skin and both hands became blue and painful in cold weather. However, these reactions were more marked in the hand treated by the application of cold.
Other methods of releasing peripheral vasoconstrictions are, (a) by applying heat to the body as a whole, which produces a generalized dilation of peripheral blood vessels in all extremities and thus produces reflex warming (Fig. 20); (b) by the action of drugs, (such as amyl nitrate, nitroglycerin, alcohol, the salicylates and papverine) which affect directly the musculature of the blood vessel walls; (c) by the action of drugs which act primarily upon the autonomic nervous system which in turn acts upon the blood vessel walls through the medium of the sympathetic motor fibers (nicotenic acid, mecholin); and (d) injection blocking of either the peripheral nerve or sympathetic nerve trunks.
As previously stated, if any of these measures are to be effective they must be carried out before thrombosis has taken place at the arteriolar-capillary junctions. Optimum results can be anticipated if the defrosting and the release of vasospasm can be accomplished while the airman is still in flight. Chemical methods for producing relaxation would obviously have great advantages over nerve blocking procedures which require exacting surgical skill.
With this in mind, we have carried out experiments which amyl nitrate, nitroglycerin, alcohol and aspirin. These drugs were administered both to normal persons and to patients who had recently received injuries to their fingers from excessive cold. The effect of these drugs on the peripheral capillary circulation was studied by means of electric thermocouples and simultaneous direct microscopy of the capillaries themselves. Contrary to the generally accepted action as reported in text books, none of these drugs caused an elevation of the temperature in the tested parts, nor did they cause a dilation of the capillary bed (Fig. 19).
Similar experiments with drugs acting upon blood vessel walls through the medium of the autonomic nervous system have also been carried out with similar negative results.
REFERENCES
1. GREENE, RAYMOND. Lancet, Lond., 1941, 2: 689.2. Ibid., 1942, 2: 695.
3. LEWIS, SIR THOMAS. Vascular Disorders of the Limbs. P. 9. London: Macmillan and Co., 1936.
COMMENT
John E. Scarff, M.D
. Department of Neurosurgery, College of Physicians and Surgeons, Columbia University
I was very happy when Colonel Davis asked me to assist in his investigation of high altitude frostbite. Our studies were begun upon airmen suffering this condition who had been admitted to the 2nd General Hospital, at Oxford, where I was a member of the staff. Some very important observations were made here. But it seemed highly desirable to us both to see and study frostbitten fingers at the earliest possible moment after the injury had occurred. To accomplish this, Colonel Davis arranged with General Hawley that I be temporarily relieved of other duties, and assigned to duty at the United States Army Station Hospital serving the VIII Bomber Command Headquarters, at one of the airfields in East Anglia.John E. Scarff, M.D
. Department of Neurosurgery, College of Physicians and Surgeons, Columbia University
My reception at the bomber base, not only by the medical staff but also by the tactical staff, was extremely cordial, for these men were all well aware of the seriousness of high altitude cold injuries, not only to the individual airmen but to the overall operation of Bomber Command. The commanding officer promised me every possible assistance, and more than made good on his promise. I was allowed complete freedom of the bomber base at all times. I was invited to attend all of the premission briefings. I was allowed to go out with the rescue crews meeting the damaged planes as they returned from combat missions; to inspect, at will, the planes after they had returned, to see the nature and extent of the damage they had sustained from enemy gunfire; to inspect the oxygen equipment and the electrically heated suits of the gunners, to see what damage they had suffered; and to select for immediate hospitalization those airmen I thought showed early signs of frostbitten fingers or toes. I was allotted a generous number of hospital beds in a single ward and my own small but well equipped laboratory on that ward. I was introduced and welcomed at the Flying Officers' Mess, and made a temporary member of the Flying Officers' Club, both of which provided me wonderful opportunity to discuss the high altitude frostbite problem with the men actually faced with it. I was even permitted to fly in all practice missions, although not on combat missions, in order that I might see at first hand the actual conditions encountered by the various airmen during flight. In brief, my reception could not have been more cordial, nor the cooperation tendered me more complete.
Our first undertaking was to set up a complete, systematic daily census of all airmen with frostbite injuries. This quickly confirmed Colonel Davis' initial impression of the high incidence of this type of injury among the Air Force personnel.
Our second undertaking was to make detailed description and photographic documentation of all cases of high altitude frostbite injuries, supplementing those already begun at the 2nd General Hospital, and thus establish and record, for the first time in medical literature, the gross pathology of this new clinical-pathological entity.
The third undertaking was to confirm, if possible, Colonel Davis' original hypothesis that the basic pathophysiology of high altitude frostbite, principally responsible for the serious and permanent damage to fingers and toes, was an acute, intense, obstinate vasoconstriction of the peripheral arterioles of the fingers and toes, occurring as an instant reflex vasomotor response to exposure of these parts to the extreme cold of -50şC. encountered at combat altitudes of 40,000 feet, inducing prolonged ischemia and anoxia of the fingers and toes, and resulting in irreversible and permanent damage to the tissues of these parts. Microscopic examinations were made of the capillaries in the nailbeds of the fingers and toes of airmen suspected of having frostbite injury, both immediately upon their return from combat missions and at frequent intervals thereafter. These examinations consistently revealed complete absence of circulating blood in the capillary beds, and confirmed completely the correctness of the original hypothesis.
Our forth undertaking was to find a method, or methods, for quickly relaxing the intensely constricted peripheral arterioles in the frostbitten fingers and toes. An intensive and wide-ranging search was made, but no drug or technical procedure was found that would relax the constricted arterioles. In desperation, we even prescribed whiskey, ad lib., to a number of volunteers just returned from combat missions with waxy fingers, on the basis of the widespread, but false, belief that alcohol caused a flushing of the skin, resulting from dilatation of peripheral arterioles. The only results of these experiments were wards filled with completely uninhibited, extremely hilarious airmen, who created embarrassing disciplinary situations, and wails of anguish from the staff of the nearby Quartermaster's Depot, from which the whiskey had been requisitioned, who asked, "Who in hell is draining away all of that beautiful whiskey?" Nor, to our added disappointment, was any effective definitive treatment for high altitude frostbite, once incurred, ever discovered. Al of this, the gross pathology, the pathophysiology, and our futile efforts to develop an effective therapy, was reported in the December, 1943, issue of Surgery, Gynecology and Obstetrics.
Our fifth undertaking was a search for factors such as faulty equipment or faulty operational procedures that were most frequently responsible for the occurrence of high altitude frostbite injuries. Here the results were very rewarding, in that a relatively small number of faults in equipment and operational procedures were found that appeared to be consistently responsible for most of the high altitude cold injuries suffered by the airmen. Moreover, these appeared to be easily and effectively correctable. Here are some examples:
The two waist guns were fired from an unheated compartment of the plane, through wide-open windows about 4 feet square. The only protection from the intense cold for the waist-gunner was an oxygen mask, which covered only about two-thirds of the face, and electrically heated wearing apparel. At -50şC., a blast of the cold air striking these men at 200 to 250 miles per hour practically doubled their vulnerability to severe injuries from cold, should they have to remove their electrically heated gloves for even one to two minutes to unjam their guns or replace obstructed oxygen masks, both of which were frequently necessary during combat.
The brace of tail guns was located at the extreme rear end of the fuselage. The tail gunner knelt, looking aft, with his hands on the grips of these guns, his knees doubled under him, the soles of his feet pointing forward in the aircraft, toward the waist gunner's compartment, against the wall of which he frequently struck his back and especially the soles of his feet, in which the circulation of blood had already been impaired by the acute flexion of the knees. Frostbitten toes and feet were a frequent result.
True, there was a solid metal door that could be used to close the entrance from the waist gunner's compartment into the tail gunner's compartment. But no tail gunner was found, among the many interrogated, who would closet that door! With the door closed, they all suffered an acute sense of isolation from the rest of the crew, and indeed were all obsessed to varying degrees by the fear that if the ship were badly damaged, "those s.o.b.'s up front might all bail out," without telling them, leaving them alone and unaware of what was happening, to go down with the doomed ship. Quite understandably, they preferred frostbitten feet to that fate!
Each member of the bomber's crew was supplied with an individual oxygen delivery system, connecting with the master oxygen supply tank and distribution system of the plane. The individual airmen's equipment consisted of a molded rubber face mask covering his nose, mouth, and part of his cheeks, connected by a narrow rubber tube to a soft rubber bag that acted as an intermediary oxygen reservoir, inflating and deflating with each respiration, similar to the bags used in administering nitrous oxide-oxygen anesthesia. This in turn was connected by a long rubber tube to a fixed outlet of the ship's master oxygen supply system, located on the wall of the compartment.
The rubber tube leading from the face mask to the inflating-deflating rubber bag containing the fresh oxygen was too small in caliber, with the result that when the warm, moisture-laden air exhaled by the waist gunners passed through this narrow tube, chilled to -50ş C. by the cold air encountered at altitudes of 40,000 feet, the moisture in the exhaled breath promptly condensed as ice on the inner wall of the tube, gradually narrowing its lumen until complete closure occurred. When this happened the gunner quickly had to replace his original oxygen delivery system with a second emergency unit, with which he was supplied, to prevent acute general hypoxia.
The very act of replacement, however, presented the airman with another serious hazard, namely, frostbitten fingers. The oxygen masks then being supplied the airmen were held to the face by means of a very badly designed head harness that was easy to manage with ungloved hands, but was almost impossible to handle when the thick and stiff electrically wired gloves were worn. As a result, whenever the first oxygen mask froze, the airman had to remove both of his heated gloves for a minute or two in order to replace the original mask with the emergency mask, a long enough exposure of his bare hands to the intense cold of combat altitudes, to set off an acute vasospasm of the terminal arterioles in the fingers, and initiate the pathological sequences of high altitude frostbite.
The electrically heated suits, gloves, and boots were all wired together in series, that is, by means of a single continuous electric circuit, like the old fashioned Christmas-tree lights in which failure of a single light bulb caused all the light bulbs to go out. In the original flying suits, if the electric circuit was broken at any single point in the suit, in either glove, or in either boot, all five pieces of wearing apparel would immediately become cold, and remain so throughout the remaining two or three hours of the mission; this complication occurred quite frequently.
The possibility of this complication was aggravated by the habit of the waist, tail, and belly gunners, after the combat phase of the mission was over, and the bomber began to descend to lower altitudes where the air was warmer, to congregate in the waist gunner's compartment and take off their heavy, hot, sweaty electrically wired suits and drop them onto the floor. The floor of the waist gunner's compartment by that time would be covered to a depth of 2 to 3 inches with the empty brass shell casings that had been ejected from the waist guns while they were being fired. The gunners would walk back and forth on top of these electrically wired suits, which would be crushed between the heels of the airmen's leather boots and the knife-sharp edges of the spent brass shells, and frequent breakage of the fine electric wires within the suits resulted. A single break in the electrical wiring of any one piece of this electric wearing apparel - suit, gloves, or boots - caused complete failure in all five pieces of equipment, and if it was undetected, the suit would be useless on the next mission.
After the return of a bomber squadron from a combat mission, a clean-up squad would pick up the discarded electric suits, gloves, and boots, usually wet with sweat, from the floor of the waist gunner's compartment, return them to the squadron rooms, and dump them on the floor in piles, where they would remain until reissued the following morning to the airmen setting forth on a combat mission.
There was no provision for drying the suits before they were reissued. There was no routine testing of the intactness of the wiring, or of the electric connections between suits, gloves, and boots, before they were reissued; in fact, there was no electrical connection or outlet in the squadron rooms that would accept the electric connections to the suits, nor indeed any electric current comparable to that produced by the electric generators on the plane itself. The electric suits could be tested only in the plane after the planes motors were running; therefore, breaks in the wiring of the suits, gloves, and boots were frequently not detected until after the planes had taken off on a combat mission, too late for repair or replacement of the defective suits.
The individual airmen were never issued their own personal suits, gloves, or boots, with their names conspicuously stamped or sewn on each item; they felt none of the sense of personal responsibility for the care of the suits that comes from knowing that this same specific equipment would be reissued to them each time they set off on a combat mission. Instead, the electrically heated apparel was simply taken off the tops of the piles and issued in a first-come, first-served manner. Many times gloves or boots issued were too small for comfort, and even too small to permit good circulation of blood in fingers and toes; but these facts might not be realized until after the bombers were on their way.
In general, the airmen disliked wearing oxygen masks, and so would delay using them until they became conscious of oxygen shortage. As a result, there were often periods of one to two hours during the long climb from sea level to the 40,000 foot combat altitude when the airmen were continuously hypoxic, at times even severely so, just short of respiratory decompensation but without conscious distress. However, these subclinical levels of hypoxia, especially when prolonged for one to two hours, greatly lowered the resistance of finger and toes to injury during even brief, necessary exposure to the excessive cold of high altitude.
The frequent existence of this prolonged state of severe although subclinical hypoxia was brought to our attention by the oft-repeated story of the belly gunner. As a rule, the belly gunner would let himself down through a small trap door in the floor of the waist gunner's compartment into his Plexiglas gun turret, soon after the plane had begun to climb toward combat altitudes. There he would sit, doubled-up in a fetal position, completely immobile and comfortable, often dozing during one to two hours of the climb to combat altitudes. But about the time the plane was reaching an altitude of 30,000 to 40,000 feet, the belly gunner would feel the need to empty his bladder before the ship began to "mix it up" with the enemy. To do this he had to pull himself up through the trap door, into the waist gunner's compartment, and walk about 10 feet to a pee hole in the side wall of the fuselage. It was not uncommon for the belly gunner to pass out cold when he undertook to do this. Subsequent questioning would usually reveal that the belly gunner had not been wearing his oxygen mask up to that time, and for the preceding hour or two had probably been in a state of severe although subclinical hypoxia that had been progressively lowering the resistance of all of his tissues to any insult. But, because he had been experiencing no subjective symptoms, except perhaps a slight drowsiness, the belly gunner had not bothered to don his oxygen mask. Nonetheless, the oxygen level in his blood had become so low that the slightest physical exertion resulted in complete clinical decompensation.
It was eventually established that not only the belly gunners but in fact most of the airmen delayed putting on their oxygen masks until they became consciously aware of air hunger, and hence were experiencing a relative, but sometimes severe, hypoxia for at least an hour while the plane was climbing to combat altitudes. This prolonged hypoxia greatly lessened the resistance of the tissues of their hands and feet to the injury incurred by even the briefest exposure of ungloved hands to the intense cold of high altitudes, which frequently was necessary for unjamming the machine guns, among other reasons.
Our sixth and final undertaking was to formulate some recommendations for the correction of the faults in Air Force equipment and procedures that we had found. A list of recommendations was submitted to General Hawley for his transmission of the Air Force:
Installation of Plexiglas turrets for the two waist guns.
Replacement of the solid metal door between the waist gunner's compartment and the tail gunner's compartment with a transparent Plexiglas door.
The use of a rubber tube of larger caliber to connect the oxygen face mask to the flexible rubber oxygen bag, and the use of a simpler head harness, similar to that used on a baseball catcher's mask, to hold the airman's oxygen mask to his face.
Replacement of the airman's original electrically heated suits, gloves, and boots, wired in series, by new equipment, wired in parallel.
The issuance of personal and properly fitting electrically heated suits, gloves, and boots to each airman, with his name plainly marked on each item, at the beginning of his tour of flying duty; and improvement in the system of collection, drying, electrical testing, and reissuance of these personal items of equipment to the individual airmen at the start of each mission.
That a specific altitude be established, upon recommendation of the Air Force Medical Staff, above which it would be mandatory for all airmen to wear their oxygen masks.
On a Sunday morning in August, 1943, General Arnold, accompanied by General Grant, Surgeon General of the United States Air Force; General Grow, Chief Surgeon of the Air Force, European theater of operations; General Hawley; and Colonel Davis visited the 2nd General Hospital at Oxford, England, to see the 100 or so hospitalized airmen of the VIII Bomber Command suffering from high altitude frostbite. A data sheet for each airman, giving his name, rank, serial number, and squadron number, the date and mission on which the frostbite injury had been sustained, and the circumstances responsible for the injury, had been prepared. General Arnold spent several hours interrogating the individual airmen, verifying the facts stated on the data sheet, and personally inspecting the injured hands and feet, until he was satisfied with the accuracy of Colonel Davis' report regarding the high incidence of, and great disability resulting from, high altitude frostbite, as well as the justification for, and reasonableness of, the recommendations contained in the report.
Following General Arnold's return to Washington, a number of changes in airplane equipment and Air Force clothing were effected by the Quartermaster Corps, largely through the efforts of a civilian friend of Colonel Davis, Mr. Henry Field of Chicago, who personally brought all of our material before the Quartermaster General.
In addition, the Air Force requested from Colonel Davis, and were granted, permission to reproduce in large posters the photographs showing various stages and degrees of high altitude frostbite injuries to airmen's hands that had originally been published in the December, 1943, issue of Surgery, Gynecology and Obstetrics. The format for the poster was designed by us. The Air Force then had this poster printed in large quantities, and distributed for prominent hanging in all of the squadron rooms of the bomber commands, as a constant reminder of the dangers incurred by even brief exposure of hands to the freezing cold air of high altitudes. A four-page pamphlet on the same subject describing the condition, contributory factors, and precautionary measures was also prepared by us, at the request of the Air Force. This was printed in large quantities by the Air Force, and distributed to every member of their bomber commands.
As a result of these combined efforts by the Air Force and the Army Medical Corps, both originating from Colonel Davis' initial recognition of the new syndrome and its importance to the Air Force, the occurrence of high altitude frostbite among the airmen of the VIII Bomber Command progressively lessened; by December, 1943, airmen suffering from this condition had become almost a rarity. Assuming that the 100 airmen suffering from disabling high altitude frostbite who were found in various Army Hospitals and brought together at the 2nd General Hospital at the time of General Arnold's visit represented the average number of airmen grounded each week because of frostbite, and projecting this weekly average for the 100 weeks remaining before V-E Day, one can estimate that approximately 70,000 flying days of highly trained, highly motivated combat airmen of the VIII Bomber Command were saved as the result of the high altitude frostbite study originated and directed by Colonel Davis.